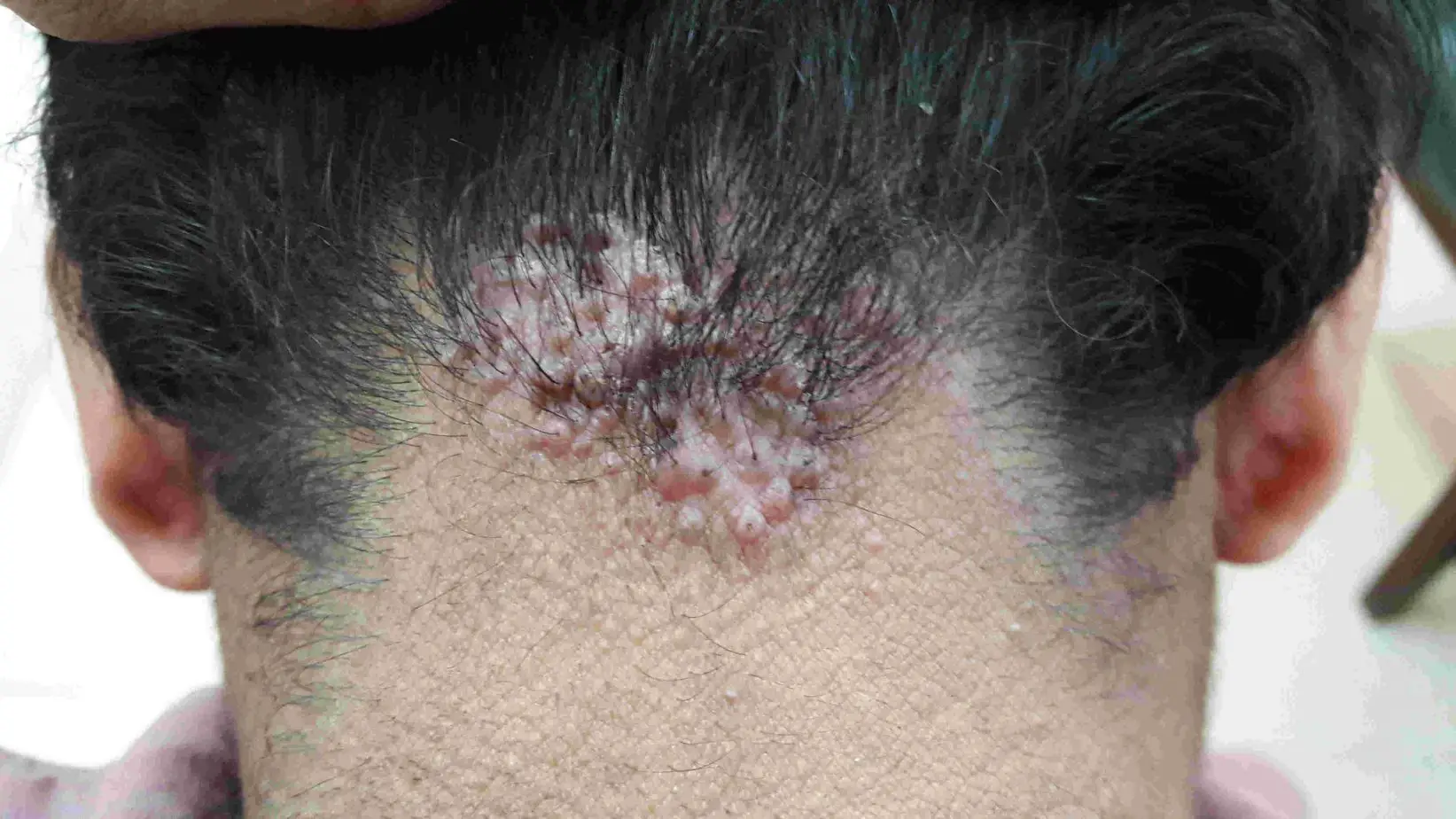
Acne Keloidalis is more of an inflammation and infection than a type of acne. As a result, it does not go away or disappears on its own without treatment. It first appears as itchy grains in the nape area of your neck. Gradually, the itch becomes intense, and the area becomes red and irritable.
The hair on and around the itchy area falls off, and it becomes unsightly. Unlike ordinary acne, however, keloidalis won’t leave on its own, and is in fact, difficult to treat. Different techniques can be used to treat acne keloidalis; however, the result varies in people.
What Is Acne Keloidalis?
Acne keloidalis nuchae is a condition identified by pustules and papules that forms on the scalp and neck. Although it bears the name acne keloidalis, the condition does not occur due to acne vulgaris. Instead, it is a type of folliculitis.
Folliculitis is an infection or inflammation that affects the hair follicle, the small cavities around the hair roots. Since it affects the hair follicle, the condition occurs in different places where hair grows. However, it is most common on the scalp, neck, and other places where friction takes place.
Acne keloidalis is a skin condition that affects the back of the scalp. At inception, it appears as pus-filled or red bumps that may either be tender or itchy. If left untreated, the bumps may enlarge and form keloids or scars. In severe cases, the condition may also cause hair loss.
While the exact cause of acne keloidalis is unknown, it is believed to be linked to tight-fitting collars, helmets, or other gear that rubs against the back of the neck. Treatment options include medicated shampoos, creams, and steroids. In severe cases, surgery may be required to remove the scars.
Acne keloidalis appears like a rash or small bump. Sometimes it can be chronic. As time passes, the small itchy bumps develop into scars, and hair falls off the follicle. When the scars enlarge, they appear like keloids and are usually raised and tough.
Does Acne Keloidalis Nuchae Go Away?
Acne keloidalis is not a type of acne, and it does not go away on its own. The condition is difficult to treat, and the available treatments only ease the symptoms.
In some cases, the condition can go away but only for a short while. It is likely to come back after some time.
Acne keloidalis is a chronic condition, and it can last for months or years. The symptoms might go away and come back from time to time. However, the scars might remain even after the condition has resolved.
Acne keloidalis is a condition that requires treatment. If you have the condition, you should see a doctor to find out the best treatment option for you. There is no sure way to prevent the condition, but you can take some steps to reduce your risk of developing it.
How Do You Treat Keloidalis Acne?
Electrosurgery
Electrosurgery involves cutting through tissue with a high-frequency electric current. Hence, instead of using a scalpel as in the case of other surgical procedures, it uses electricity. As expected, the procedure is also much neater and faster.
Surgical Excision
On the other hand, surgical excision is the contrast of electrosurgery. It is a type of traditional surgical procedure that involves using a scalpel to cut the lesion. It is mostly used to treat large lesions to prevent regrowth. The surgical wound may take weeks or months to heal; however, it heals best if left open.
Laser Therapy
Like surgery, different laser therapies are used to treat acne keloidalis. For example, laser hair removal is ideal for treating mild cases. Light or laser therapies work by destroying the hair follicle and decreasing inflammatory response. Hence, it is more like attempting to root out the problem than surface treatment. However, laser therapy takes time, and the sessions can spread over a few weeks.
You should treat any infection or underlying condition before beginning the therapy. In some cases, doctors sometimes combine retinoids and topical steroids with the therapy for significant results.
Medications
Medications don’t offer the most promising result for acne keloidalis. However, doctors sometimes recommend a combination of medications to treat the condition. For example, steroid injections work for large papules, and topical steroids can be prescribed for smaller ones. Doctors may also prescribe oral corticosteroids for inflamed and large lesions for a short period and take oral antibiotics to prevent infections.
One thing, though, you shouldn’t try self-medication since the condition is not like one you see every day. Instead, discuss possible treatment and procedures with your doctor.
Over-The-Counter Treatments
Your doctor can recommend some over-the-counter products to help the treatment and prevent acne keloidalis from growing worse. The commonest prescriptions include shampoo and soap. Coal tar shampoo and keratoplastic drugs are used to treat itchy skin conditions. They are also ideal for causing the skin to grow new skin cells and shed dead ones. Plus, they offer relief from itchiness and scaling.
Besides treating acne keloidalis, you also need to prevent further infections. To do this, doctors recommend antimicrobial cleansers and soap for use in the affected area. The soaps sometimes contain benzoyl peroxide, chlorhexidine, etc. However, be sure to follow the instruction on the frequency and period of use.
In contrast to what many believe, acne keloidalis does not just go away. However, although there is no known cure, your doctor can try a combination of treatment options to prevent further triggers.
Surgery
Severe acne keloidalis appears with large scars that, in severe cases, may even require surgery for removal. The surgical options depend on the severity; some of the options include surgical punch, electrosurgery, and surgical excision.
Surgical punch or skin punch is performed using a circular, hollow blade to puncture the skin to remove the lesion. Also referred to as a punch biopsy, the operated area is stitched closed after treatment with anti-inflammatory medication.
What Causes Acne Keloidalis Nuchae?
There is no clear-cut definition of what causes acne keloidalis. However, some studies have shown that it occurs more in certain people and parts of the body. For example, it is common in men with curly, short, or stiff hairs. Some of the notable causes include:
Close Shaving And Irritation
An injury from using a razor during a close shaving is linked to acne keloidalis. This is because shaving injuries can destroy the hair follicles or cause the hair shafts to irritate the hair follicle walls. When the walls are irritated, it can result in inflammation, and the resulting inflammation can destroy the follicle and leave a scar.
Apart from this, constant friction and irritation caused by wearing helmets and tight shirt collars can also cause acne keloidalis. The reason for this is because tight wears like helmets tend to pull on the hair and cause scarring through folliculitis.
When you shave too close to the skin, the sharp, curved hair is directed back into the skin and can prompt an inflammatory response. The friction caused by shirt collars makes the condition worse since humidity and heat does not help.
Medication And Genetics
There have been cases of individuals developing acne keloidalis after using certain medications. For example, cyclosporine and some antiepileptic drugs have been linked to the skin condition. The genetic mutation also increases the chance of acne keloidalis since the genes play a significant role in the structure of the hair follicle.
Chronic Infection
The most significant cause of acne keloidalis is chronic and low-grade infections. Folliculitis is often caused by fungi or staph bacteria. Both can be contacted through contact with contaminated items or from secondary infection to the site.
What Are The Symptoms?
The symptoms of acne keloidalis are easy to spot. The first sign is the appearance of small, firm bumps on the back of the neck near the hairline. The bumps progress to pus-filled pimples and eventually turn into hard, thick scars.
In severe cases, the scars can become so large that they distort the shape of the ear or affect the function of the ear. The scars can also make it difficult to wear glasses or headphones.
How Do You Get Rid Of Bumps On The Back Of Your Neck?
Acne keloid is most common at the back of the neck and the lower back of the scalp. At inception, it appears as pus-filled or red bumps that may either be tender or itchy. However, the bump develops into tiny scars that can transform into large or thick scars if not treated. An advanced form of acne keloidalis is associated with a foul-smelling discharge from the affected area.
The best way against Acne Keloidalis is to keep it at bay by using best skin hygiene habits. However, if it has occurred, it would help to keep the following in mind.
Try Simple Home Remedies
Gently wash the affected area with a non-irritating cleanser and wash. However, don’t scrub too hard to avoid irritating the site any further.
Apart from this, you shouldn’t wear a shirt with collars that rub against the back of your neck.
If you participate in sporting activities, you should avoid wearing sports helmets and other tight-fitting gears that will rub your neck.
More importantly, though, do not shave close to the back of your neck.
However, keep in mind – do not deploy any self-help remedy unless you are completely sure about it. Because poorly informed self-help measures can cause more harm than good. Instead, seek medical help.
Seek Medical Help
Home remedies and management tips cannot replace medical treatment. When you suspect you have acne keloidalis, seek help from a dermatologist or local care provider to prevent the formation of a larger scar. In the worst case, the formation might cause hair loss in the affected region. Your physician may prescribe any of the following treatment for your acne:
- Topical creams, gels, and lotion: Retinoid creams like tazarotene, adapalene, and tretinoin are examples or retinoid creams that your dermatologist may prescribe. In other cases, it could take an antibiotic like clindamycin or a prescription-strength steroid.
- Oral medications: antibiotic pills and short steroid courses like prednisone are handy for treating severe and advanced acne keloidalis cases.
- Surgical removal: in the worst case, your dermatologist may recommend a surgical procedure to remove or reduce the scar tissue. For example, he can inject steroids directly into the inflammation or use surgical excision to remove larger scars or single bumps. He could also try laser destruction or the liquid nitrogen technique.
The bottom line is that acne keloidalis can be managed if detected early. If detected early, your dermatologist can prescribe treatments to prevent the scar from transforming into something much worse. In essence, you should seek medical care early.
How To Prevent Acne Keloidalis Nuchae?
The best way to prevent acne keloidalis is by practicing good hygiene habits and by maintaining a healthy lifestyle.
Some of the tips you can follow to reduce your risk include:
- Wash your hair regularly and avoid touching or scratching the back of your neck.
- Avoid sharing personal items like hats, towels, combs, etc. with others.
- Avoid wearing tight-fitting collars, helmets, or other gear that rubs against the back of your neck.
- If you participate in sports, shower immediately after and wash your hair to remove sweat and bacteria.
- Use a medicated shampoo or cream if you have a history of scalp infections.
- Be sure to consult a dermatologist if you have any concerns about your risk of developing acne keloidalis. Early detection and treatment are key to preventing the condition from worsening.
Conclusion
Acne keloidalis has a good prognosis if you start treatment early. However, it does not mean you won’t have to deal with associated pain and discomfort. Although it is not related to typical acne, it is more typical in young men of Asian, Africa, and Latino descent. This is not to say it can’t be found in women; however, cases of occurrence in women are extremely rare. Plus, it is rarely seen in people before puberty or after middle age.
In this series: